When novel drugs or medical devices are evaluated in clinical trials, the data generated in this process is called clinical data. Improving the use of technology in clinical trials is now a prime opportunity for the life sciences industry. Digital trial processes enable us to automate operational decisions, which in turn can improve efficiency and site-centricity. A typical data journey could begin with data being captured on paper at a site, before entry into EDC, streaming into a safety system, and then being included in a monitoring report on adverse events, for example. Technology should be able to identify which scenarios require source verification, almost as soon as the data enters the system. By connecting user experiences to data flows, different teams can come together at the source, creating new opportunities for trial acceleration.
DIGITAL TRANFORMATION IN CLINICAL TRIALS
The most recent digital transformation has led to predominant use of electronic data capture (EDC) software over standard paper case report forms (CRFs). Moreover, the variety of new digital software that facilitate more efficient, reliable and fast clinical data collection (such as electronic Consent (eConsent) electronic Patient Reported Outcome (ePRO), electronic Clinical Outcome Assessment (eCOA) emerge at high-speed nowadays.
WHAT IS CLINICAL DATA MANAGEMENT?
The term “data management” refers to a wide range of practices and methodologies employed for the purpose of helping Sponsors better leverage their data. Typically, data management practices make use of a combination of processes, including:
- Data collection—integrating data sources in an organized manner, to enable the organization to derive value from the data.
- Data access—implementing strategies that enable organizations to create, update, and access data across various data tiers, including archives.
- Data storage—building storage strategies that leverage as many data storage types as needed, including multi cloud, private and public clouds, and on-premise storage.
- Data availability—implementing backup and disaster and recovery plans that ensure business continuity during various disaster scenarios.
- Data security and privacy—enforcing security and privacy policies on a continual basis.
The main goal of data management is to ensure that data remains a secure, private, and accessible asset, generating actionable insights for the organization.
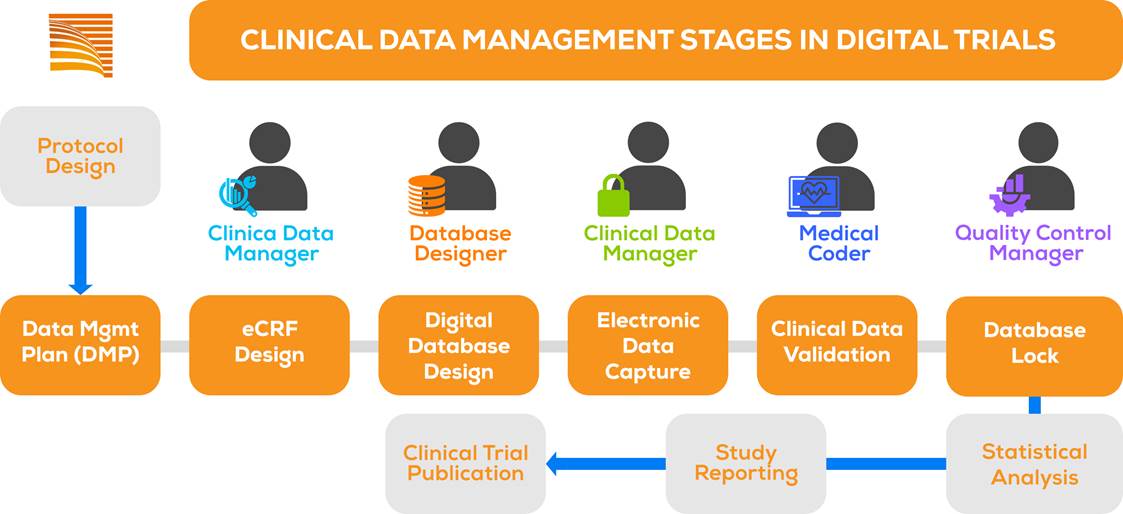
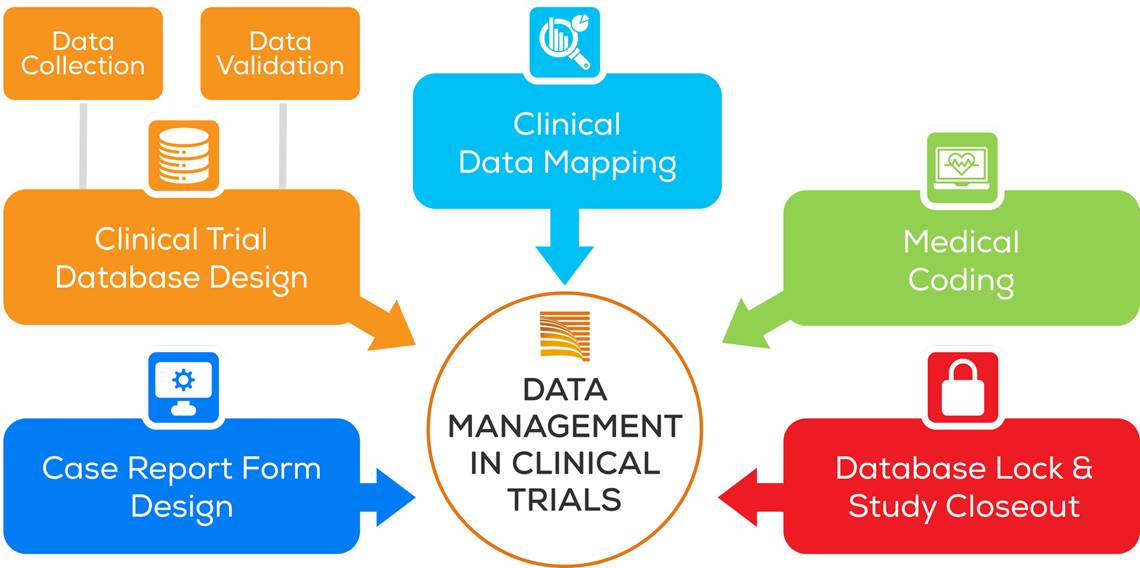
CLINICAL DATA MANAGEMENT STAGES
The document detailing all data management procedures is commonly called the Data Management Plan (DMP).
We illustrate the essential elements developed in the DMP through the following brief outline:
- The purpose of the activity to be performed;
- Definition of responsibilities;
- Guidelines and standard operating procedures (SOPs) to be applied;
- Type of documentation/outputs to be generated;
DATA MANAGEMENT PLAN (DMP)
Data management is a critical business driver used to ensure clinical data is acquired, validated, stored, and protected in a standardized way. It is essential to develop and deploy the right processes so end users are confident their data is reliable, accessible, and up to date.
The DMP may include elements derived from other study documents so that the DMP comprises a complete documentation of the whole clinical study. On the other hand, the DMP can also record only key information with references to appendices and other separate documents for details. Both of these procedures are reasonable and meet the need of consolidating data management activities.
CASE REPORT FORM DESIGN CONSIDERATIONS
Paper case report forms (CRFs) or electronic case report forms (eCRFs) are developed in accordance with clinical protocol requirements.
It is recommended not to repeat the same questions during the design of eCRFs. however, some important measures can be double-checked within eCRFs with questions that ask the same question but in different ways (“logical integrity check”). In addition, eCRF questions should not allow blank spaces. Another consideration is that if the answer is not available for a field, it is recommended to answer: NA (not applicable), ND (not done) or UNK (unknown).
CRFs also include pages that can have an important impact on data flow, during the eCRF processing phase. These are longer comments or free text, analog diagrams or scales, log-type forms for adverse events (AEs), patient questionnaires, and early termination pages.
It is important to note that this type of design of special eCRFs requires special attention from the data manager, as the way these data are collected will substantially affect data output and subsequent analysis.
It is a good idea to have a team of CRF experts carefully review each page and sign off on the eCRF design.
STUDY SETUP
The study setup includes creating a database and preparing the study for clinical data entry into the validated EDC software. Study setup also requires annotated CRFs and a design document for specifications (optional). When the EDC platform has been developed, it is ready for testing, which usually takes place in the development environment. A tester must answer the following questions:
- Is data stored in the correct field?
- Are the calculated values calculated, and correct?
- Are all hidden variables filled in as required?
- Is any data truncated or improperly stored?
- Are there inappropriate blank records?
ENTERING AND CLEANING DATA
Modern electronic solutions for data capture have substituted a double entry of data which was commonly used on paper CRFs, dramatically reducing the error rate while entering data. Inserted data can be modified, although regulatory standards require audit trails to store all the changes made to clinical data, and those changes should be available for the audit trail any time. Some data inconsistencies that require research are called discrepancies. In other words, discrepancies that are sent to the site for the following resolution are termed “queries”. Most common data discrepancies comprise missing values, simple range checks, logical inconsistencies and protocol violations. In modern EDC systems there is two types of queries – automatic (raised based on some predefined data entry condition) and manual ones (raised by monitors, clinical research associates, data managers etc). EDC systems stores such queries, tracks its status, records its resolution.
MANAGING LABORATORY DATA
Laboratory data is a data that represents various health parameters measurements, such as blood chemistry, lipids, urinary values, cell cultures, microbiology, virology and other assays specific to the protocol. Laboratory data can be manually entered into EDC system, though the importing setting might be also adjusted to make the transfer of laboratory data from specific equipment into EDC uniform and error-low. Good Clinical Practice (GCP) guidelines require that all the labs employed in a particular clinical study have full documentation, data-audit trails, respective SOPs, professional staff, archiving system of samples and data, and routine quality assurance inspections.
SERIOUS ADVERSE EVENT (SAE) HANDLING
Patients enrolled in a clinical study can have some undesirable experiences which are called adverse events (AEs). AE form usually includes the text describing the event, start/stop date, different indicators including severity, frequency, relationship to drug/medical device and actions taken. Though, normal data entry guidelines should sufficiently cover the requirements for data entry of AE data, there might be special procedures applied that describe allowed and required changes to reported terms to facilitate coding process. In addition, AE terms are subjected to medical coding and in case of AE being defined as SAE it must be reported to respective a safety group or safety coordinator.
CREATING REPORTS AND TRANSFERRING DATA
Data reports can be categorized into two groups: standard reports are consisting of standard representation of the data that is generated over and over on one data set, while customized reports represent the reports, format and content of which are requested by user and are generated just once. The identification of what data should be included in the report or transfer one might ask three following questions: “From where,” “Exactly what,” and “When?”. Clearly answered these questions will be a good foundation for generation high quality data reports. Transferring of the data to internal or external groups also belongs to the data management activities. Because transferring of the data almost always involves safety and efficacy information, the degree of efforts dedicated to data transfer must be much higher than that for most of reports.
CLOSING STUDIES
Upon collecting the last patient’s data from all participated sites, usually comes the urge to close and “lock” the study. Eventually when the study has been locked, the final analysis of the data can begin. Since the companies are under a high to pressure to make those analysis, based on which the market decision will be taken, they are often keep a track on “time to database lock” time. This pressure to lock the study fast comes against a great deal of study closeout activities such as collecting the comprehensive data, resolving pending queries, conforming against other databases, and conducting final quality control (QC).
When these activities are performed and responsible person signs off, the clinical study is considered locked. It means that from this moment no data can be changed. In addition, one has to bear in mind that since the study is locked, there is unlikely to find any data inconsistencies, missing data etc. If here is enough of data changes or the changes are crucial, the study will be unlocked, but this requires a special procedure.
DOCUMENTING AND SOPs
For each clinical trial and related data management activities it is pivotal to prepare and to have an essential standard operation procedure (SOPs). These SOPs should cover all the elements of the data generation, collection, and validation throughout of the study. SOPs must provide enough detail to make sure that the data management activities are carried out consistently and according to up-to-date relevant regulation. Each document should include a description of appropriate materials (forms, procedures, checklists etc). SOPs related to EDC system should include the procedures for the following activities: system setup/installation, system maintenance, data backup, recovery, contingency plan, security and account maintenance and change control.
CLINICAL DATA MANAGEMENT SOFTWARE
Electronic data capture (EDC) systems transfer clinical trial data from the clinical sites to the sponsor through electronic means which makes working with data more efficient and secure. EDC systems are designed for the site activities within clinical trial and typically features eCRFs for the entry of data, single field and cross-field checks, query tools to allow raise and resolve data inconsistencies, electronic signatures and means to assist monitoring actions.
Current EDC solutions are differentiated on the basis of features that allow easier control over the data collected in the clinical stud, the level of validation and their flexibility to accommodate specific study needs. Medical image transfer may be integrated into the EDC, for rapid and secure transfer of medical imaging from a clinical site to the core lab. Data validation module helps to control data quality with smart alerts, instant compliance checks, quick data clean-up for monitors and data managers.
BEST CLINICAL DATA MANAGEMENT PRACTICES
The clinical data landscape is continually evolving. The clinical data management practices must be flexible, scalable and intelligent to keep pace with the variety, volume and velocity of data captured. Data needs to be unified to deliver a complete patient view, intelligently analyzed to identify issues, and automatically transformed to accelerate database lock and kick-start trial data analysis. When data management is undertaken using legacy approached, it is done manually. Conversely, centralizing data management creates opportunities to automate the acquisition, cleaning, and reconciliation processes—which could be considered working digitally.
The right digital strategy can empower genuine site- and patient-centricity. But its development requires us to address three challenges: localizing to patient and regulatory requirements, delivering complete and concurrent clinical data cleaning, and automating critical operations. With the right tools, sponsors can enhance the efficiency of trial execution, provide patients with new ways to participate in studies, and simplify collaboration with clinical sites.
The most advanced data capture systems allow building custom analytics, so that investigators and sponsors can make better decisions, sooner and hence more successful. In addition, it is critical to select an EDC system powered with online safety adjudication possibilities, that facilitates rapid online adjudication, accelerating the delivery of primary or secondary endpoints. Sponsors are advised to rely on data management experts to develop a robust data collection process and select an EDC system that will make the data collection in your clinical trial more secure, compliant and efficient.







Leave A Comment